Table of Contents
I. Understanding the Function of the Heart
III. The 4 Stages of Congestive Heart Failure
V. Medications for Heart Failure
Understanding the Function of the Heart
A healthy functioning heart is essential to the health of the entire body. If you are experiencing heart failure, your heart is not pumping as well as you should. This is a chronic condition that cannot be cured, but many people can live for several years after receiving a heart failure diagnosis.
Frequent medical attention and medications like Cozaar (losartan), Corlanor (ivabradine), Farxiga (dapagliflozin), and Lopressor (metoprolol) can help prevent severe heart failure symptoms and complications. Heart failure can also lead to severe edema (swelling of the body’s tissues), and diuretics like Lasix (furosemide) can help prevent these unpleasant symptoms. But how does the heart work, and why do these problems occur?
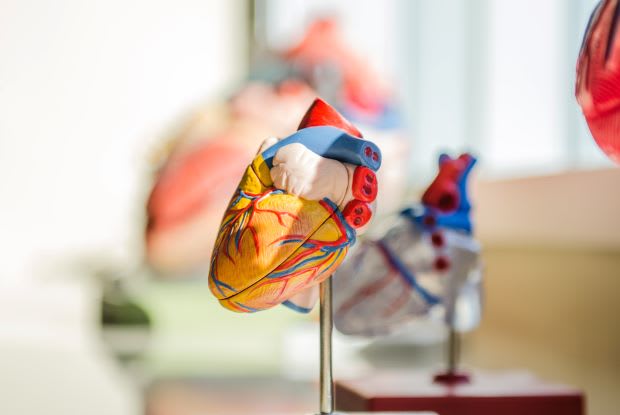
The heart has two chambers: the upper chambers called the atria and the two lower chambers called ventricles. The right atrium takes in oxygen-depleted blood from the body and sends it through the right ventricle which pushes blood to the lungs to be oxygenated. This newly oxygenated blood then travels to the left atrium and then to the left ventricle where it gets pumped to the rest of the body.
When the heart cannot pump correctly, the cells do not receive the proper nutrients and oxygen, leading to fatigue, shortness of breath, and coughing fits. Heart failure can take a massive toll on a person’s quality of living, so it is essential to avoid the risk factors that may lead to this chronic condition. [1] Read on to learn more about heart failure and treatment options.
Symptoms of Heart Failure
Heart failure varies from person to person. In some cases, heart failure can occur quickly (acute heart failure) or it may be ongoing (chronic heart failure). Heart failure symptoms may look like several other medical conditions, so a proper diagnosis is necessary before a treatment plan is made. Signs and symptoms may include:
- Lack of appetite and nausea
- Decreased alertness
- Chest pain (if a heart attack causes heart failure)
- Increased need to urinate at night
- Shortness of breath when you exert yourself or when you lie down
- Rapid or irregular heartbeat
- Coughing up pink and foamy mucus
- Swelling of your abdomen
- Weight gain from fluid retention [2]
The 4 Stages of Congestive Heart Failure
Heart failure is a chronic condition that occurs slowly over time. The stages are classified as A, B, C, and D, ranging from a high risk of developing heart failure to advanced heart failure.
a. Stage A
This is the earliest stage and is commonly referred to as pre-heart failure. Your doctor has determined that you are at high risk of developing this chronic disorder. If you have a history of heart failure in your family, you may be classified as Stage A. You are also at risk if you have the following conditions:
- Hypertension
- Diabetes
- History of alcohol abuse
- History of taking drugs that may damage the heart muscles (like cancer drugs)
- Coronary artery disease
b. Stage B
Stage B is often asymptomatic, which means that you will not display the typical symptoms of heart failure. In most cases, patients with Stage B have been diagnosed with systolic left ventricular dysfunction. This means that the heart cannot contract normally and cannot produce enough force to push the blood into circulation.
You are fully diagnosed with heart failure at this stage. The typical symptoms and side effects of heart failure are fully present and medications like Lasix and Cozaar are taken as part of a treatment plan. Heart failure patients at this point will most likely experience the following symptoms: Advanced symptoms of heart failure are present in this stage. Symptoms will not improve with treatment, so this is classified as end-stage heart failure. At stage D, you will likely have to undergo alternative treatment options like a heart transplant, heart surgery, ventricular assist devices, and palliative or hospice care. The five-year survival rate of every stage of heart failure is around 50 percent. By the tenth year of living with heart failure, the survival rate is around 30 percent. [4] As mentioned above, there are two stages of heart failure that may not present symptoms. This is why it is important to get a yearly physical, especially if heart problems are common in your family. If a close relative has been diagnosed with heart failure, you are at an increased risk of developing heart failure yourself. Do not try to diagnose yourself and seek emergency medical help if your symptoms become severe. If you have high blood pressure, coronary artery disease, or diabetes, your doctor will perform more intense procedures to check for heart failure. Echocardiogram: This test creates a video image of your heart, which can help determine the shape of the heart and any abnormalities. Echocardiograms also measure the ejection fraction, showing how well the heart is pumping blood in and out. Electrocardiogram (ECG): The heart's electrical activity is measured by attaching electrodes to the skin. The heart rhythm is measured through this test and can help detect an abnormality. Stress test: A stress test involves being hooked up to an ECG machine while you perform physical activity like walking or jogging on a treadmill. You may also have to wear a mask that measures the ability of your heart and lungs to take in oxygen and breathe out carbon dioxide. Treating heart failure is a multi-faceted process and often requires several medications. If you have high blood pressure caused by lifestyle choices like poor nutrition or a smoking habit, you are at a greater risk of heart failure. Along with diet and exercise changes, you will likely need at least two medications to treat this condition. If you want to save money your heart medicine, visit our online Canadian pharmacy. The types of medications can include: Angiotensin II receptor blockers: These drugs widen the heart's blood vessels, lowering blood pressure and improving blood flow. Drugs like Cozaar (losartan) can decrease the workload of the heart and reduce heart failure symptoms. Beta-blockers: Lopressor (metoprolol) is a beta-blocker that slows your heart rate and reduces blood pressure. It may also lessen damage to the heart if you have been diagnosed with systolic heart failure. They can regulate the heart rhythm and lessen the chance of sudden death. Diuretics: These medications are also known as water pills. Diuretics like Lasix (furosemide) may be prescribed to decrease fluid accumulation in the body, especially the lungs. Heart failure creates fluid collection in the body, and using Lasix can lessen the fluid on the lungs so you can breathe easier. Other medications: Upon diagnosis, your doctor will create the right combination of medications. Farxiga (dapagliflozin) is one prescription that has multiple uses. It can be used for type 2 diabetes, heart failure, and chronic kidney disease. In heart failure patients, it can reduce the risk of cardiovascular death and hospitalization, especially in heart failure patients who also have type 2 diabetes. [5] Corlanor (ivabradine) is another drug used for systolic heart failure and reduces the heart rate and lowers blood pressure. Ivabradine also affects the heart’s electrical activity to slow the heart rate. [6] When taken properly, these medications can hopefully prevent heart failure from worsening. Sometimes medications are not enough, and you may require more serious medical intervention like a VAD (ventricular assist device) or heart transplant. A VAD is a mechanical circulatory support device that helps pump blood into the ventricles. These implants are placed in the abdomen or chest and attached to the weakened heart. A heart transplant is the last resort for heart failure. If you get on a list for heart transplants, you will likely continue taking medications to improve your symptoms and maintain your quality of life. You may have to wait a long time before a suitable donor is found. Your doctor will determine if a transplant is a good option for your heart failure. The content in this article is intended for informational purposes only. This website does not provide medical advice. In all circumstances, you should always seek the advice of your physician and/or other qualified health professionals(s) for drug, medical condition, or treatment advice. The content provided on this website is not a substitute for professional medical advice, diagnosis, or treatment.
c. Stage C
d. Stage D
Diagnosing Heart Failure

Medications for Heart Failure

