Table of Contents
I. Understanding Fungal Infections
II. Risk Factors for Complications
Understanding Fungal Infections
The majority of the time, fungus on the skin does not cause any complications, but sometimes unpleasant conditions may occur. Superficial skin infections most commonly affect the nails, skin, hair, and warm, moist areas of the body, including the feet and groin. Most people inhale fungal spores or come in contact with spores without much consequence, but others with weakened immune systems can develop infections.
Common fungal skin infections like athlete’s foot, ringworm, jock itch, and yeast infections are typically not serious and can be treated quickly. If your infection is not clearing up quickly, you may be prescribed antifungal medications like Lotriderm cream (clotrimazole/betamethasone), Vermox (mebendazole), Spectazole (econazole), Diflucan (fluconazole), and Oxistat cream (oxiconazole). Many people think that their infections will clear up on their own, but you may be putting your body at risk of dangerous complications if you do so. Read on to learn more about possible complications of fungal skin infections. [1]
The immune system is essential in protecting the body from infection, and several disorders can weaken this system and make you immunocompromised. Immune disorders can range from mild to severe. 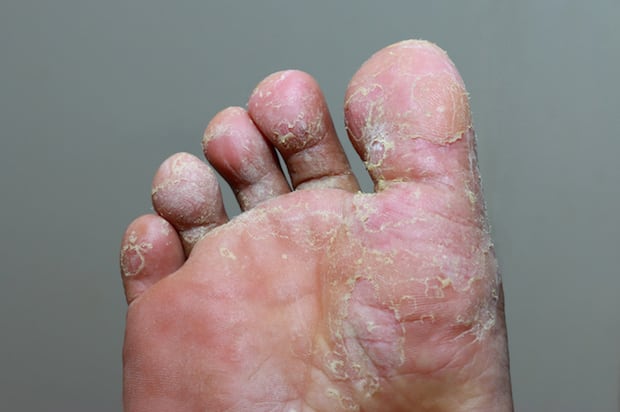
Risk Factors for Complications
Get savings updates for Diflucan
As mentioned briefly above, having immune conditions can increase your risk of developing a dangerous fungal infection complication. [2] Common immune disorders or situations that may make you more prone to fungal skin infections include:
- HIV/AIDS: HIV and AIDS attack the immune system and destroy the cells that normally fight infections.
- Taking steroid medications: Steroid medications reduce inflammation in the body but may reduce the immune system's activity by affecting the way white blood cells function.
- Undergoing chemotherapy: Chemotherapy targets rapidly dividing cells, destroying cancer cells as well as healthy cells. Chemotherapy medicines can damage the bone marrow, affecting red blood cells, white blood cells, and platelets. [3]
Abscesses
There are many types of fungal skin infections, but all of them involve some form of skin redness and cracking. All of these symptoms can lead to abscess formation. Fungal skin infections occur in warm, moist areas of the body covered with clothes or shoes, making it difficult for the infection to dry out and heal.
If the infection remains for a long period of time, an abscess may occur. An abscess is a collection of pus underneath the skin when an infection is trapped in the body. White blood cells flock to infections on the body to treat the infections, causing pus to form. Pus contains living and dead bacteria and white blood cells that were killed or injured by the infection. Skin abscesses can form anywhere on the body. Symptoms include:
- Peeling or ulcerating skin
- Redness, warmth, or swelling
- Oozing or drainage of fluid from the skin [4]
Nephritis
If you have HIV, AIDS, or hepatitis and develop a fungal skin infection, you are more likely to develop nephritis. Nephritis affects a structure called nephrons, which is a functional unit in the kidneys. Nephritis, also known as glomerulonephritis, occurs when nephrons become inflamed and affect kidney function.
Nephritis can be dangerous because the kidneys are essential in circulating blood and removing excess water and waste from the body. You may develop acute glomerulonephritis if you develop a severe infection like strep throat, hepatitis, or HIV. You need prompt medical care if you suspect nephritis. Warning signs may include: Endocarditis is a serious condition that leads to an inflammation of the heart’s chambers and valves. This condition occurs due to infection caused by bacteria, fungi, or other germs that may enter the bloodstream and attach to damaged areas in the heart. If your fungal skin infection gets out of control, the infection may enter the bloodstream and cause an infection in the heart. People with damaged heart valves, artificial heart valves, and heart defects are at a higher risk of endocarditis. It is essential to treat your fungal skin infection with the proper antifungal drugs like Lotriderm cream (clotrimazole/betamethasone), Vermox (mebendazole), Spectazole (econazole), Diflucan (fluconazole), and Oxistat cream (oxiconazole) to prevent this serious complication. Endocarditis usually occurs slowly, and symptoms vary from person to person, depending on your previous heart conditions. Common symptoms of endocarditis include: Fungal meningitis is rare in the United States but can still occur if a fungal infection spreads to your lungs, brain, or spinal cord. Candida is one fungus that is known to enter the bloodstream and affect internal organs. Symptoms of fungal meningitis may include: For most people, Candida can live outside the body and on the skin with no issue, but if a fungal skin infection occurs, it may enter the body through cracked or broken skin. Other fungi that can cause meningitis include: The content in this article is intended for informational purposes only. This website does not provide medical advice. In all circumstances, you should always seek the advice of your physician and/or other qualified health professionals(s) for drug, medical condition, or treatment advice. The content provided on this website is not a substitute for professional medical advice, diagnosis, or treatment.
Endocarditis

Fungal Meningitis
